Case Of The Week
Bipolar Hip Arthroplasty
Jan 2024

Dr. Mahesh Vidhani
Specialist Orthopedic Surgeon
Visit Profile
Book Appointment
Reason for Admission
The patient , a 76-year-old lady, who was a visitor from London presented at Emergency department with history of fall while walking on the road on 20/12/2023. Following that she was unable to stand and walk, with severe pain left hip joint.
Diagnosis |
Transcervical Fracture Of Neck Femur Of The Left Hip.
The patient was sustained transcervical fracture neck femur of left hip. She was admitted for arthroplasty left hip under my care. On detail history taking she was found to be a case renal transplant, twelve years ago. She was on immunosuppressant drugs and steroid tablets for long duration. She was also on Plavix (clopidogrel), as she had developed renal vein thrombosis more than twelve years ago. She was referred and consulted at this hospital by cardiologist Dr. Rahul, Nephrologist-Dr Ahmad, Internist Dr. Deepak Dube and Anesthesiologist Dr. James Donato.
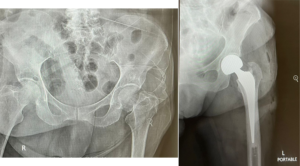
On 22/12/2023, she underwent – Bipolar arthroplasty of left hip successfully, with utmost asepsis care.
Postoperatively she underwent physiotherapy. On next day of surgery, she was able to stand and walk with full weight bearing, with aid of walking frame. She was discharged from hospital on 03/01/2024, on the same day flight she went back to London.
Discussion
This case was unique because she was a case with tendency for venous thrombosis, because of her previous history, so she could not be kept long in bed more than few days that requires early surgery with fracture hip, otherwise she would likely develop deep venous thrombosis. On the other hand as she was on clopidogrel, that requires delayed surgery with risk of excessive bleeding as ideally we wait 5-7 days after stopping, the clopidogrel to avoid excessive bleeding.
So with this dilemma, of risk of developing thrombosis vs excessive bleeding she was taken for surgery after 48 hours of stopping clopidogrel, with preparation of preoperative blood transfusion and standby three more blood transfusions ready, also two units of platelets were kept standby in case excessive uncontrollable bleeding was encountered during surgery.
During surgery about 50 percent more bleeding was encountered than usual with such procedure, 300 ml, which was controlled by careful hemostasis with cautery, and fine dissection and using cemented implant. Post operatively 12 hours after surgery she was put on clexane to avoid post operative venous thrombosis.
More over as she was on immunosuppressants and steroids for long duration, she was on risk of developing postoperative infection with prosthesis in place risk gets amplified for this reason utmost asepsis care was taken preoperatively.
She went home, recovered fully without any complications because of careful planning and implementation of management protocol.
Dr. Mahesh Vidhani
Specialist Orthopedic Surgeon