Breastfeeding is one of the foundations of child health, development and survival. For these reasons, the World Health Organization (WHO) recommends that infants should exclusively breastfeed for the first six months; meaning no food or drink other than breast milk is offered to breastfeeding baby for up to 6 months. Baby is fed on self-demand, day and night with no restrictions on the length or frequency of breastfeeding. Complementary foods can then be introduced, with continued breastfeeding until 24 months of age or older.
Breastfeeding has been known to have several advantages that make it ideal—benefits of breastmilk span not only for children but also mothers.
Benefits of breastfeeding for children
-
- Breastmilk provides all the energy and nutrients that the infant needs.
- It is safe, clean and contains antibodies which help protect against many common childhood illnesses.
- Breastfed children perform better on intelligence tests, are less likely to be overweight or obese and less prone to diabetes later in life.
- Reduce the risk of allergies, rickets and Anaemia.
- Readily available, with no preparation and suitable to child’s need.
Benefits of breastfeeding to mother
- Promotes mother and child bonding.
- It prevents uterine bleeding in the mother after delivery.
- A natural form of Family Planning.
- Reduces the risks of breast and ovarian cancer in the mother.
- Saves time and precious expenses need not be used for buying milk powder and health care.
Due to all numerous benefits, breastfeeding counselling should give to all pregnant women in the early antenatal period.
Nevertheless, contraindication to breastfeeding does exist. Some of them include:
- HIV, HLTV 1 & 11 infections. (Adult T-cell lymphoma virus)
- Active Tuberculosis.
- Herpes lesions on the mother’s breast.
- Infant with Inborn error of metabolism; galactosemia, phenylketonuria.
- Mothers on certain medications; anticancer therapy, radioactive isotope etc.
However, the success of breastfeeding depends on proper breastfeeding technique; the key of that is adequate latching. While breastfeeding one must keep check of the mother’s position:
- The mother can nurse sitting or lying down
- The mother should be in a comfortable and relaxed positionable to hold the baby close to her without undue effort, her feet be supported
The technique of breastfeeding also entails the infant’s position to be in check:
- The baby’s head and body must be perfectly lined up
- The baby’s face must face the mother’s chest, with his nose in front of the nipple
- The baby’s body must be close to the mother’s, turned towards her
- If the baby is newly born, the mother must cradle him with one arm and give support to the buttocks, not just to the head and shoulders
Another vital characteristic to keep in check is the Infant attachment to the breast:
- The mouth is wide open
- The chin touches the breast (or close to)
- The lower lip turns outwards
- More areola is visible above the infant’ top lip
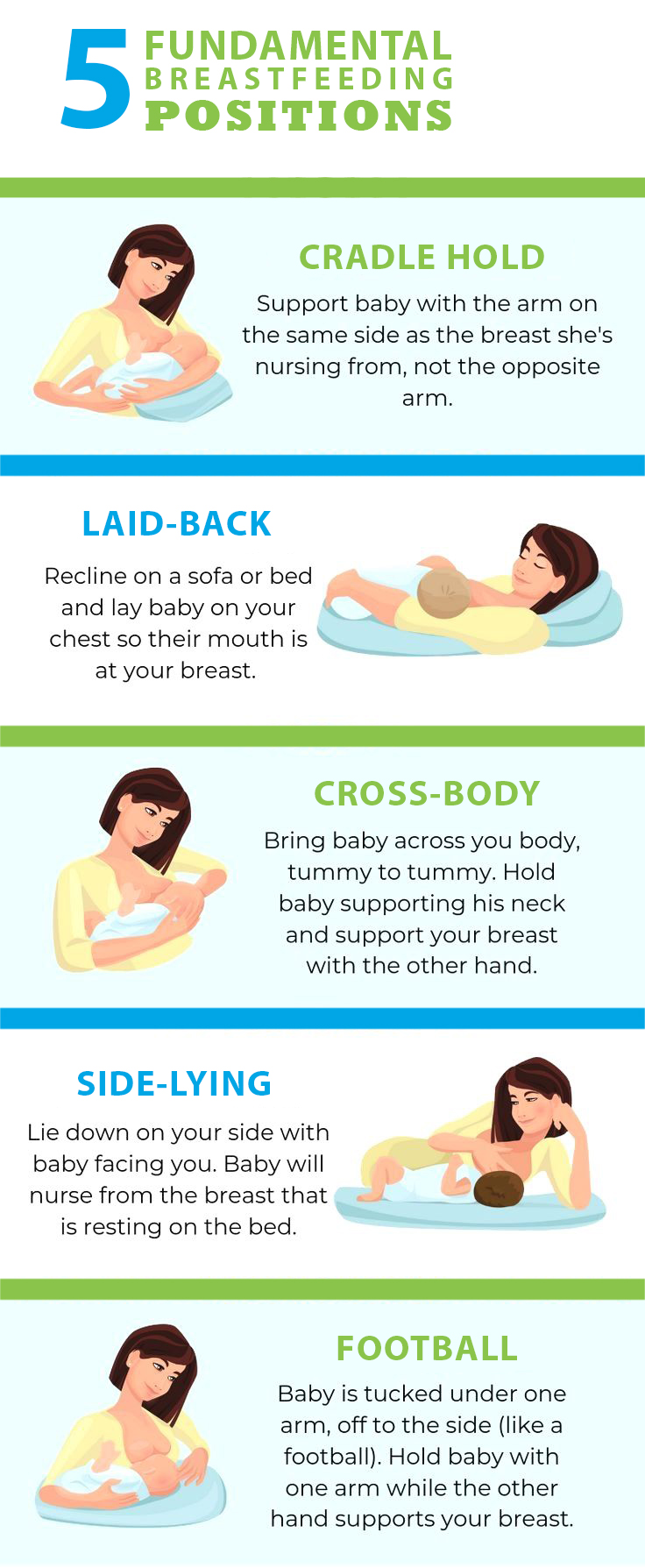 There are many positions that a mother can use to achieve all the criterion required for effective breastfeeding, as mentioned above. However, the best positions can be separated into five categories that are mentioned in the picture provided below.
There are many positions that a mother can use to achieve all the criterion required for effective breastfeeding, as mentioned above. However, the best positions can be separated into five categories that are mentioned in the picture provided below.
Even though the techniques of breastfeeding are essential, a mother must make sure that effective breastfeeding is taking place to ensure the baby’s health and development. The signs mentioned below will allow the mother to conclude if the infant is appropriately nurtured.
Signs of Effective Breastfeeding
- Frequent feedings 8-12 times daily.
- Intermittent episodes of rhythmic sucking with audible swallows should be heard while the infant is nursing.
- Infant should have about 6-8 wet diapers in 24 hours once breastfeeding is established.
- Infant should have a minimum of 3-4 bowel movements every 24 hours.
- Stools should be about one tablespoon or larger and should be soft and yellow after day 3.
- Average daily weight gain of 15 -30g.
- Infant has regained birth weight by day 10 of life.
Sometimes, a mother may encounter barriers to effective breastfeeding that are caused due to:
- Lack of confidence in mother;
- Belief that breast milk is not sufficient;
- Lack of adequate support system;
- History of previous breast surgery;
- Breast engorgement, cracked and sore nipples;
- Retractile nipples.
Another method of breastfeeding is through expressed breast milk.
Indications include:
- Preterm / sick baby
- Working mother
Storage of Expressed breast milk
- Clean wide-mouthed container with a tight lid
- At room temperature 8-10 hrs.
- Refrigerator – 24 hours, Freezer – 20° C – for three months
In conclusion, breastfeeding infants is the best way to ensure their growth and health. With mothers ensuring that proper techniques are used for effective breastfeeding, it can be concluded to be the most effective tool in the child’s development. Mothers are encouraged to ask the help of their Obstetrician or Pediatricians to understand the best techniques for breastfeeding infants.
Breastfeeding is a mother’s gift to herself, her baby and the earth.
-Pamela K. Wiggins.